Hysterectomy
Hysterectomy, the surgical removal of the uterus, is a recommended intervention in variety of gynecologic conditions, including:
- Abnormal excessive bleeding
- Fibroids
- Uterine cancer
- Cervical cancer
- Endometriosis and adenomyosis (in some cases)
These are just a few of many conditions that might require a hysterectomy.
Typically, depending on whether the condition is benign (such as fibroids or pain) or malignant (such as cancer), either a total hysterectomy with the removal of the body of the uterus together with the cervix, or subtotal/partial hysterectomy (the cervix is left behind) is performed. Removal of the ovaries at the time of hysterectomy is very controversial topic and should be discussed individually in every case.
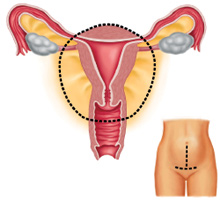 In the past, the only available option for hysterectomy was an open abdominal surgery. The incision would be made in either "bikini" or up-and-down fashion, the uterus would be removed, and abdomen closed in multiple layers with sutures and staples.
In the past, the only available option for hysterectomy was an open abdominal surgery. The incision would be made in either "bikini" or up-and-down fashion, the uterus would be removed, and abdomen closed in multiple layers with sutures and staples.
Typically, a woman would spend 2 to 3 days in the hospital with several months of recovery at home. In addition, the surgery would leave a large scar on the abdomen.
Laparoscopic Hysterectomy
Utilizing magnified surgical field and available electrosurgical and ultrasonic instruments, the removal of the uterus is achieved through several (usually 3 to 4) ½ to ¼ inch incisions. Minimal blood loss and fast recovery time are the major advantages of laparoscopic hysterectomy, not to mention excellent cosmetic results. Most women go home either the same or next day and fully on their feet within a week or two.
Robot-assisted laparoscopic hysterectomy (RALH) utilizes the same laparoscopic principles combined with the improved visualization of the surgical field and enhanced manipulation of robotic instruments.
The robotic surgical system provides surgeons with enhanced true 3-D vision, ergonomic comfort of surgical manipulation and unprecedented precision of tissue handling. Utilizing the EndoWrist instruments of the daVinci Surgical system, the surgeon is capable of performing precise, fine-tuned movements of robotic arms with "7 degrees of freedom," eliminating tremor and allowing for instrument manipulation that would be impossible in conventional laparoscopy.
Typical incisions in the robot-assisted laparoscopic surgery
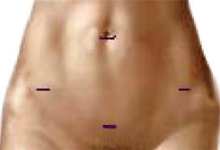
These are the few of the benefits of the robotic hysterectomy:
- Decreased blood loss
- Faster recovery time
- Greatly reduced post-operative pain
- Quicker return to daily activities
- Improved cosmesis
For More Information
To make an appointment, please call 667-214-1300 or 866-608-4228.

