Essential Tremor Patient Gets FUS Treatment
Golf is a favorite past-time for John Crowe. But a tremor that made his hands shake wildly made it difficult on the green.
“Putting could be the worst,” says Crowe, 78, who received a diagnosis of essential tremor almost 50 years ago. “I had to get the heaviest putter I could and then hope the ball would make it in the hole.”
While not as well known as Parkinson’s disease, essential tremor is the most common movement disorder, affecting an estimated 10 million Americans. It’s thought to be a hereditary nerve disorder that originates in the thalamus area of the brain, often causing uncontrollable shaking in the arms and hands.
“Some people can’t even drink a glass of water without holding it in two hands,” explains Howard Eisenberg, MD, a professor and the chair of the Department of Neurosurgery at the University of Maryland School of Medicine and a neurosurgeon at the University of Maryland Medical Center. “Essential tremor can absolutely impact someone’s life, and it can even be devastating. Imagine not being able to use a spoon or even type on a smartphone.”
But today, Crowe’s hands no longer shake. He received a new, noninvasive treatment called MRI-guided focused ultrasound (FUS) at the University of Maryland Medical Center. It is one of only a handful of hospitals in the country that offers FUS for essential tremor.
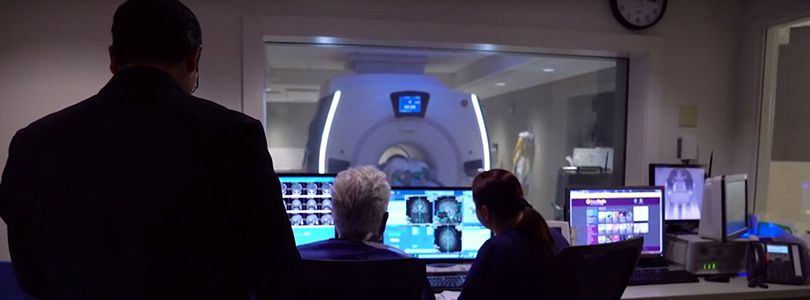
How FUS works
Crowe was diagnosed with essential tremor in his 20s; it affected every facet of his life. As the owner of a small business, Crowe relied on his secretary, who wrote everything for him except his signature. He developed the habit of signing his name with simple scribbles.
He found ways to live with his disease. He would lower his head to the table to eat soup. He’d get his friends to shuffle and deal during regular card games. He was prescribed medication, too, but it lost its effectiveness.
“I was embarrassed around other people,” says Crowe, who lives in Baltimore’s Federal Hill neighborhood. “You’re picking up something, and your hand is waving and shaking from the tremor, and someone sees you and waves hello. And you think, ‘I’m not saying hi to you!’”
Then a friend called to tell him he’d seen a commercial about a new study that involved treating essential tremor with focused ultrasound. Crowe was intrigued.
FUS uses detailed brain imaging and heat-generating sonic waves to pinpoint and kill brain cells associated with the essential tremor. More than 1,000 sonic waves are directed at a precise spot in the brain, traveling through the skull. The sonic waves must reach the target at the same exact time for the procedure to work.
“It’s a bit of a race, and you have to make it a dead tie,” says Dr. Eisenberg.
To make sure the waves hit the correct spot associated with the tremor, radiologists use magnetic resonance imaging (MRI) to create a map of the brain and pinpoint the target. Once it’s confirmed that no other parts of the brain will be affected, the temperature of the sonic waves is turned up to kill the targeted cells.
During treatment, the patient is awake and interacting with the care team. Patients experience a 50 to 60 percent reduction of the tremor, allowing for a greater quality of life—even for those whose tremor was not correctable with the best medicines.
“It’s noninvasive, it’s real-time and it produces a really good result. Patients come in with tremors and they leave without having any surgery, and their tremors are significantly diminished,” says Elias R. Melhem, MD, a professor and the chair of the Department of Diagnostic Radiology and Nuclear Medicine at the University of Maryland School of Medicine, who oversees the brain’s imaging during FUS with colleague Dheeraj Gandhi, MBBS.
Paul Fishman, MD, PhD, a professor of neurology at the University of Maryland School of Medicine, says there have been close to 800 cases worldwide using FUS to treat brain conditions with no reports of bleeding or infections. Patients who undergo FUS can have side effects, such as changes in sensation in the hand or problems with balance, but these issues are rarely serious.
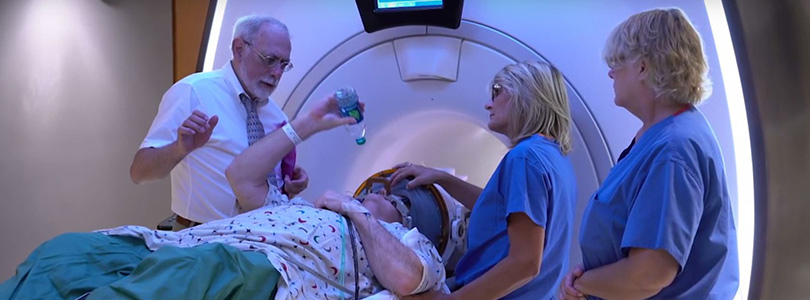
Improving on an invasive surgical option
Essential tremor can be treated medically using propranolol, but patients develop tolerance to the drug, and the effects diminish over time. Deep brain stimulation (DBS), a highly invasive treatment, has been the standard of care over the past 15 years if medications are unsuccessful.
With DBS, neurosurgeons drill a hole into the skull so a cylinder can be inserted in the brain. Through that cylinder, electrodes are implanted in the thalamus. The electrodes are connected by wires that run under the skin to a pacemaker, which is inserted in the chest. The pulsing electrodes can be modified at any time to change the effect on the tremor, and they can reduce the tremor by 60 to 70 percent.
“DBS was one of the greatest developments in neurology and neurosurgery in the last 20 years,” says Dr. Fishman. “The idea that you can modulate brain activity with an implantable electrode and have that be clinically useful—we’re talking about 150,000 people who have had this procedure done, so you know that’s clearly the standard of care.”
DBS patients also need future surgeries to replace the batteries. But many, like John Crowe, are turned away by the wires coming out of the head to the chest. He says he would sooner deal with his symptoms than undergo DBS.
“When my doctor started mentioning drilling in my head and putting wires in, I said I can live without that,” Crowe says. “And then when they came up with focused ultrasound, I thought, ‘You know what? Let’s try it.’”

The right fit, the right procedure
Once Crowe learned more about focused ultrasound, he contacted his daughter, a research associate at a local hospital, and found his way to the University of Maryland Medical Center, where he was told he was a candidate for the new treatment.
After a series of baseline tests—using a pen to go through a circular maze, drawing horizontal lines and sipping out of a lidded cup—it was finally time to have the procedure. It lasted about three hours, and Crowe heard one quick, loud bang when the sonic waves reached the cells in his brain that caused the tremor.
“It’s pretty dramatic to see the results,” says Dr. Eisenberg. “Patients can become emotional because there is such a noticeable difference right away.”
It was certainly immediate for Crowe.
When he repeated the baseline tests, he could trace the marker through the maze without hitting the sides, draw a horizontal line and drink out of a cup without spilling.
“I was tickled to death,” Crowe says.
But it wasn’t until a hospital dinner of chicken, mashed potatoes and peas that night that it really sunk in.
“I picked up the fork, picked up some peas and put them in my mouth,” says Crowe. “I never gave it a second thought until after I’m eating the chicken and I’m thinking to myself, ‘I ate those peas without them falling all over the place.’
“That was the most amazing thing.”
